After you take a breath, that vital air travels through your lungs and into your bloodstream, where it fuels every cell in your body. The amount of this life-sustaining gas in your blood is known as your blood oxygen level. It’s important to keep it within a healthy range for your body to work as it should. When levels drop too low, the effects can be serious, even life-threatening.
Measuring these levels accurately is key, especially for those managing respiratory or cardiovascular conditions. The two common methods, which are pulse oximetry and the arterial blood gas (ABG) test, offer different approaches, each with its unique strengths and limitations.
What’s Blood Oxygen Level?
Think of it as the measure of how much oxygen is flowing through your body at any given moment. This gas is the fuel your body runs on. It keeps everything working smoothly, from your brain to your heart, and even the simple act of thinking relies on it. When you breathe in through your nose or mouth, it travels to your lungs, then slips into your bloodstream and journeys to every cell you have. Those cells use it to produce energy, which powers all your daily functions, whether it’s digesting lunch or running up the stairs.
After your cells have used it up, they release carbon dioxide, which hitches a ride back through your bloodstream to the lungs so you can breathe it out. Your body is constantly working to keep these levels within a healthy range, because when they drop too low, something called hypoxemia can put a strain on vital organs, especially your brain and heart. In short, balanced oxygen levels are a sign that your lungs and circulation are doing their jobs well.
Pulse Oximetry
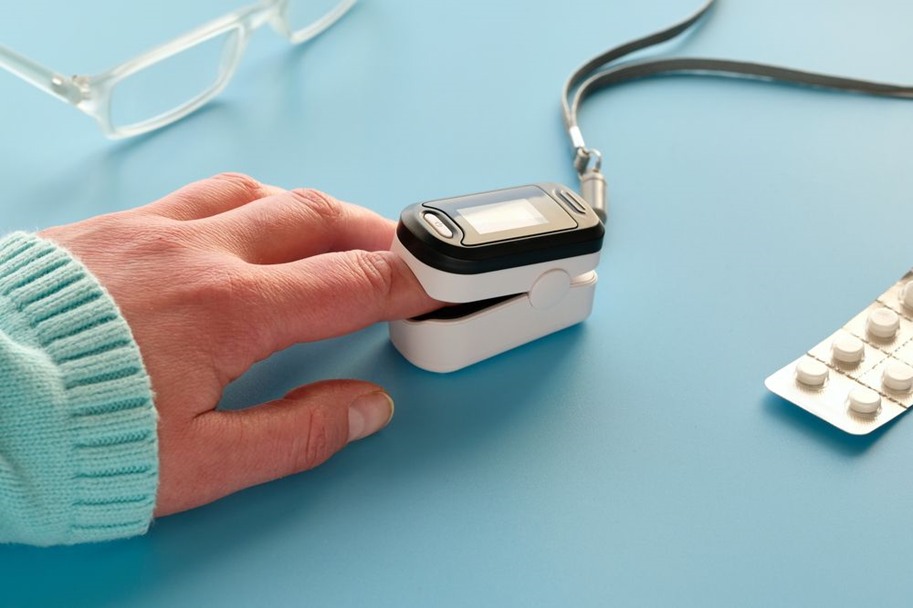
One of the simplest ways to keep an eye on your blood’s oxygen levels is with a portable pulse oxygen meter. This handy little device usually clips onto your finger or toe and quickly shows you what percentage of your blood is carrying this essential gas, along with your heart rate. While it doesn’t give the detailed information that a full blood test does, it’s a fast, painless, and non-invasive way to see if your levels are where they should be.
Pulse oximeters are used all the time in hospitals, but they’re also easy to use at home. You can pick one up at a pharmacy or online, and they’re especially useful if you want to monitor your health during a cold, after a workout, or if you have a condition that can affect circulation. Checking your levels with a pulse oximeter gives you a quick snapshot of how well your body is transporting this gas, and it can be reassuring to see a normal reading, or alert you to seek medical advice if it’s unusually low.
Blood Draw Test
Another way doctors can check how well your body is getting the air it needs is through an arterial blood gas test, often called an ABG. This isn’t just about finding out how much of this gas is in your blood, but it also measures carbon dioxide levels and looks at the pH balance, which shows if your blood is leaning too acidic or too alkaline. That balance is important because even small shifts can affect how your body works. The test involves drawing blood from an artery, which can give a more detailed picture of your overall respiratory health than a simple finger clip reading.
Why Should I Do a Blood Oxygen Level Test?
Sometimes, your doctor might suggest a blood test to see how well your body is getting the air it needs. This is usually done when something more serious is going on or to make sure the ongoing treatment is working the way it should. Here are some situations where checking your levels can be especially important:
- Sudden trouble breathing, whether you’re an adult or a newborn;
- Injuries to the head or neck that could affect how you breathe;
- Illnesses like COVID-19 or pneumonia;
- Exposure to carbon monoxide or smoke;
- Ongoing vomiting or severe nausea;
- A suspected drug overdose;
- Chronic conditions such as asthma, COPD, or cystic fibrosis;
- Heart problems that might affect circulation.
How to Increase Oxygen Level
Boosting these levels doesn’t always require medical intervention. Sometimes, simple lifestyle changes can make a noticeable difference. Spending time outside, going hiking, or letting fresh air into your home helps your body take in more air with every breath, naturally improving circulation.
Quitting smoking is another game-changer. Within a few weeks, your circulation often improves, and breathing becomes easier, which in turn helps your blood carry more of the air it needs. Even practicing basic breathing techniques, like deep belly breaths or pursed-lip breathing, can open up your airways and support better intake.
You can even use a pulse oxygen meter at home to see how these habits are helping. That said, these tips aren’t a replacement for professional care. If you have a serious underlying condition, such as pneumonia or exposure to harmful gases, these natural approaches might not be enough.
Test Details
If you’ve ever wondered how doctors check how well your lungs are working, one common way is through a simple reading with an oximeter. This small device slips over your finger and gives a quick snapshot of your blood’s saturation levels, which is something you can even do at home.
But there’s also a more detailed test that involves taking a sample of blood directly from an artery, usually in your wrist. This one is a bit more involved, often done by a respiratory therapist, and it’s part of what’s called an arterial blood gas test. Because arteries sit deeper than veins and have more nerves around them, the process can be a little uncomfortable, and some people feel light-headed during it.
Before the sample is taken, your provider might do a quick circulation check called an Allen test to make sure the blood flow in your wrist is normal. If you’re on supplemental air support, they may briefly turn it off to see how you manage on room air alone, though that’s only done if it’s safe for you. The sample is then processed quickly, giving a clear picture of how well your body is absorbing and using air.
